AACG Risk Assessment Tool
Step 1: Current Medications
Select any systemic or eye medications currently in use.
Step 2: Anatomical Factors
Identify physical traits known to increase narrow-angle susceptibility.
Your Risk Profile
Based on current inputs
Key Symptoms to Watch:
- Severe eye pain
- Colored halos around lights
- Mid-dilated pupil
- Nausea/Vomiting
Your eyesight can vanish in less than a day because of a medicine sitting on your nightstand. It sounds unlikely, but Acute Angle-Closure Glaucoma a sudden spike in eye pressure blocking drainage pathways remains one of the fastest ways to lose sight permanently. While many people associate glaucoma with old age or genetics, a significant number of cases happen after taking standard medications for allergies, asthma, or depression.
This is not a slow decline like typical open-angle glaucoma. We are talking about an event where the internal pressure of the eye shoots past normal levels within hours. If you have narrow angles in your eyes, which many people discover only during an attack, certain chemicals can trigger a mechanical blockage. Understanding the specific drugs involved and recognizing the warning signs could save your sight forever.
The Mechanics Behind the Pressure Spike
To understand why a pill causes blindness, you need to see how fluid moves in your eye. Inside every eyeball, a liquid called aqueous humor constantly circulates to nourish tissues. Usually, this fluid drains through a mesh-like structure known as the trabecular meshwork. When that exit route gets blocked, pressure builds up rapidly behind the retina.
Drug-induced AACG occurs when medications alter eye anatomy temporarily, forcing the iris against the cornea.Most attacks follow a mechanism called pupillary block. Certain drugs make your pupil dilate, or widen. In an eye with a naturally narrow channel between the iris and the cornea, a dilated pupil pushes the edge of the iris into the drainage angle. Imagine closing a door so tightly that water cannot escape; the water fills the room until the walls burst. That is what happens to your optic nerve under extreme pressure.
Clinical data indicates intraocular pressure typically exceeds 21 mm Hg during these events, often climbing to between 40 and 80 mm Hg. Normal pressure hovers around 10 to 21 mm Hg. Once pressure stays above 40 mm Hg for more than 24 hours, permanent damage becomes highly likely. You might notice a mid-dilated, fixed pupil that does not react to light, along with swelling in the clear front layer of the eye called the corneal edema.
Identifying High-Risk Medications
You might assume glaucoma only comes from eye drops, but systemic medications absorbed into your blood can trigger the same reaction. Medical reviews show that several common drug classes account for the majority of induced cases. Before starting a new prescription or buying over-the-counter remedies, check the label for these specific ingredients.
| Medication Class | Specific Examples | Risk Mechanism |
|---|---|---|
| Anticholinergics | Tropicamide, Amitriptyline, Diphenhydramine | Causes pupil dilation and iris swelling |
| Adrenergic Agents | Phenylephrine, Ephedrine, Epinephrine | Directly contracts muscles to close drainage angles |
| Serotonergic Antidepressants | Paroxetine, SSRIs, Tricyclics | Affects fluid balance and muscle tension in the eye |
| Sulfonamides | Acetazolamide, Topiramate, Sulfadiazine | Causes ciliary body swelling leading to anterior rotation |
Phenylephrine is a frequent culprit found in nasal sprays and eye whitening drops. Research suggests it is responsible for roughly 35% of documented drug-induced cases. Even antihistamines taken for seasonal allergies carry risk; first-generation types like diphenhydramine possess strong anticholinergic properties. Newer alternatives like loratadine generally pose fewer risks for the eyes but checking with a specialist remains wise.
Patients must be particularly cautious during routine eye exams. Eye doctors often use tropicamide drops to widen pupils so they can examine the back of the eye. While essential for diagnosing retinal issues, these drops can precipitate an attack in predisposed individuals. Studies indicate approximately 28% of induced cases stem from diagnostic dilation procedures rather than daily oral medicines.
Anatomical Risk Factors You Cannot Change
Not everyone who takes these medications develops acute angle-closure glaucoma. Your eye shape plays the deciding role. People with shorter axial lengths-meaning their eyeballs are physically shorter from front to back-tend to have shallower spaces between the lens and the cornea. This structural difference is often hereditary and present from birth.
Ethnicity heavily influences this anatomical risk. Asian populations, particularly East Asians, have a statistically higher prevalence of narrow angles compared to Caucasian groups. Data shows about 8.5% of Asian adults have narrow angles, whereas this figure drops to roughly 3.8% in White populations. Farsightedness, known medically as hypermetropia, correlates strongly with this shallow configuration.
Another factor is age. As the lens thickens over time, it pushes forward, further narrowing the drainage angle. This is why incidence rises significantly after age 40. Women also face higher susceptibility than men due to smaller anterior chamber depths. Despite these fixed risks, knowing you have them allows for proactive screening before taking risky drugs.

Recognizing the Emergency Symptoms
The onset is rarely subtle. Most patients describe a sudden, severe pain deep within the eye, often radiating into the forehead or nose. Unlike a typical headache, this pain feels like something pressing hard against the bone. Nausea and vomiting frequently accompany the visual disturbances because the autonomic nervous system reacts to the intense pain.
Look at bright lights during these episodes. Many victims report seeing colored rainbows or halos around streetlights and lamps. This halo effect results from corneal edema, where fluid leaks into the transparent front part of the eye, scattering incoming light. Your vision blurs rapidly, and the affected eye may appear red with swollen conjunctival vessels.
If you notice a pupil that looks different from the other-one being larger and unresponsive-this signals a mechanical blockage in action. Some patients mistake these signs for a migraine or sinus infection, leading to dangerous delays. Misdiagnosis rates remain high in general emergency settings, with some studies showing only 38% of non-ophthalmologists correctly identifying the condition immediately.
Immediate Treatment Protocols
Time acts as the enemy here. Irreversible damage to the optic nerve can occur within six to twelve hours. Standard protocol involves lowering the pressure immediately using multiple routes. Doctors typically administer pilocarpine drops to constrict the pupil and pull the iris away from the drainage meshwork.
Intravenous mannitol provides another avenue to flush fluid from the eye. This medication draws water out of the bloodstream and pulls excess fluid from the eye tissues, mechanically reducing volume. Oral carbonic anhydrase inhibitors are often given alongside these measures to stop the production of new fluid while the pressure resolves.
Laser Peripheral Iridotomy a quick laser procedure that opens a pathway for fluid drainage prevents future attacks by equalizing pressure behind and in front of the iris.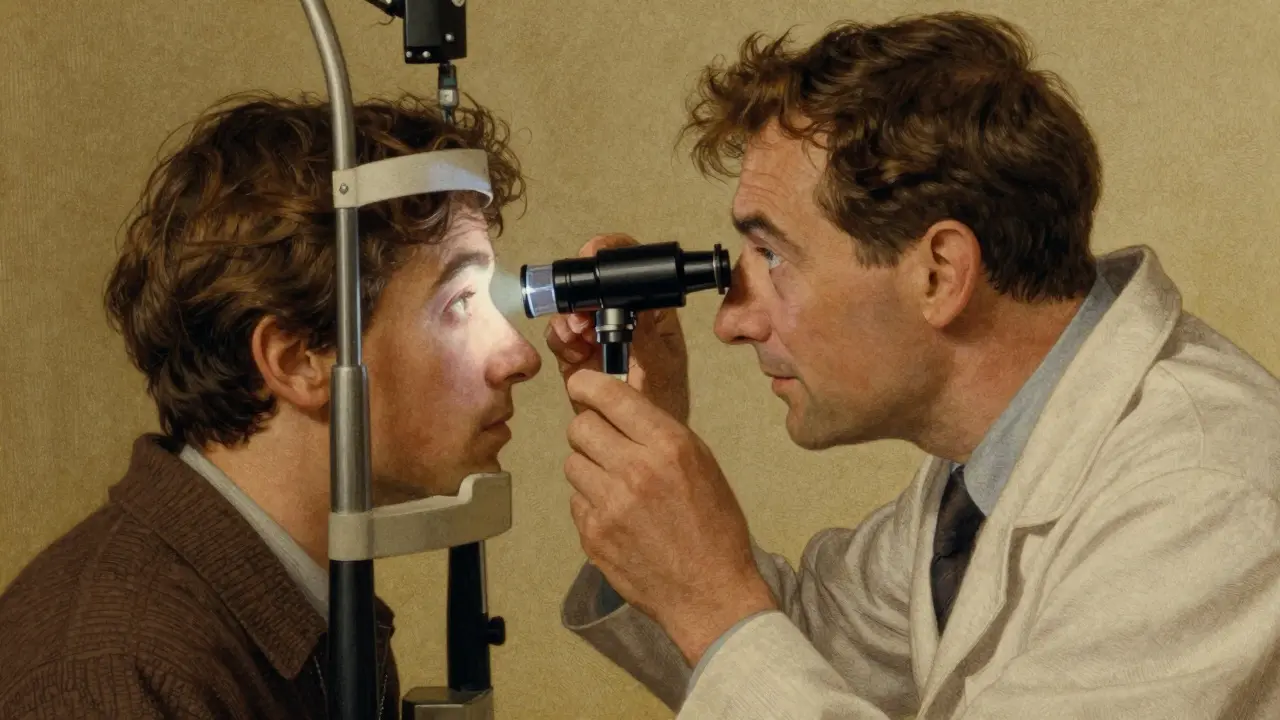
Preventing Future Incidents
Prevention relies heavily on communication. Tell every doctor you visit that you have narrow angles. If you have been diagnosed with narrow channels, carry a medical alert card or note in your wallet listing high-risk medicines to avoid. Pharmacists can flag your electronic health record to warn prescribers if they try to order contraindicated drugs.
Screening is vital for those at risk. A test called gonioscopy uses a special lens to visualize the drainage angle directly. It takes about five minutes per eye and determines if you have sufficient space. For patients over 40 with farsightedness or Asian ancestry, requesting this exam ensures safety before starting new prescriptions. Advanced imaging like optical coherence tomography offers even higher sensitivity, detecting narrow structures with 94% accuracy according to recent clinical data.
Frequently Asked Questions
Can I still take allergy medicine if I have narrow angles?
You can, but you must choose carefully. Second-generation antihistamines like loratadine or cetirizine are safer choices than older options like diphenhydramine. Always consult an ophthalmologist to confirm which specific brands do not contain adrenergic or anticholinergic compounds.
How fast does vision loss happen during an attack?
Permanent damage can start within 6 to 12 hours of symptom onset. If pressure stays above 40 mm Hg for longer than 24 hours, visual field loss is very likely. Immediate medical intervention is critical to stop the progression.
What is the difference between open-angle and angle-closure glaucoma?
Open-angle glaucoma develops slowly over years with gradual pressure increase. Angle-closure is a medical emergency where the drainage path physically closes off, causing sudden, painful spikes in pressure that require immediate treatment to avoid blindness.
Does laser surgery cure glaucoma completely?
Laser peripheral iridotomy fixes the mechanical blockage that causes acute attacks. It prevents the specific type of pressure spike associated with angle closure, but it does not treat primary open-angle glaucoma. You still need regular monitoring for other types of eye disease.
Who should get screened for narrow angles?
Everyone over 40, especially those who are farsighted, of Asian descent, or have a family history of angle-closure, should undergo gonioscopy. Screening is safe and takes very little time compared to the risk of permanent blindness.





Written by Martha Elena
I'm a pharmaceutical research writer focused on drug safety and pharmacology. I support formulary and pharmacovigilance teams with literature reviews and real‑world evidence analyses. In my off-hours, I write evidence-based articles on medication use, disease management, and dietary supplements. My goal is to turn complex research into clear, practical insights for everyday readers.
All posts: Martha Elena